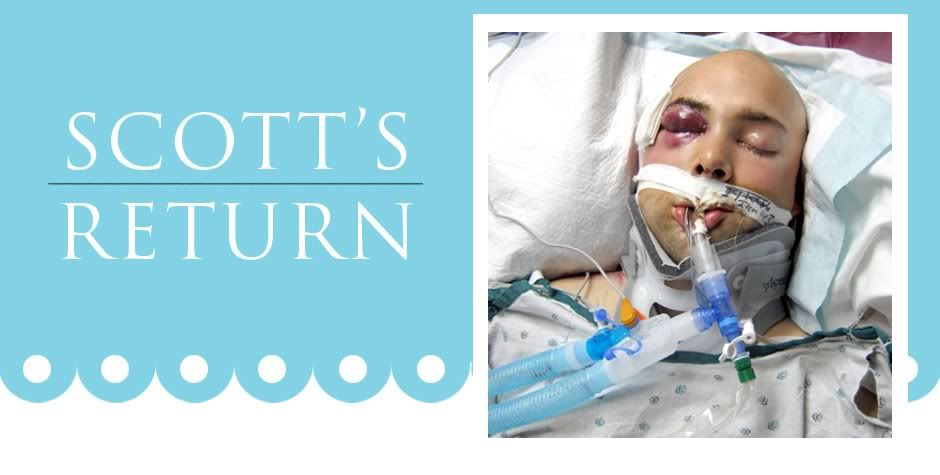
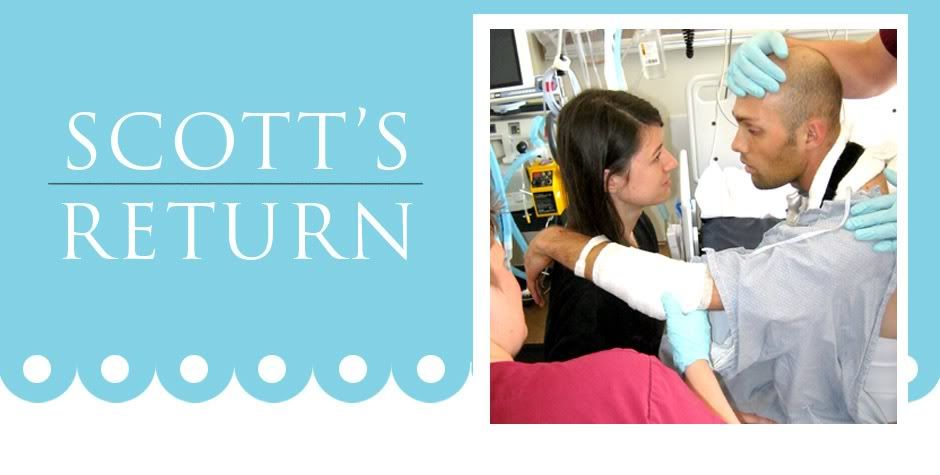
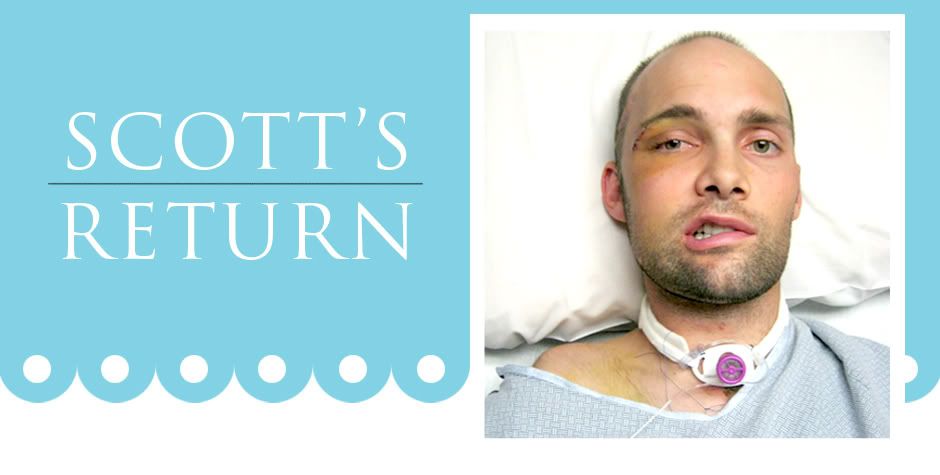
Scott’s facial surgery was successful and best of all less invasive than originally planned. Initially the physicians had diagnosed that the sinus cavities were compromised, requiring an ear to ear incision across the forehead to repair. After additional review and multiple consults, it was determined that there was no need for this repair and his sinuses would be fine. This was a huge relief for all of us as the post op recovery would be much easier with just the facial reconstruction. Scott will recover at St. Josephs over the weekend and be heading to Barrows most likely on Monday. We also hope that his trach will be removed ASAP. We fear that if the Pulmonary Physician doesn’t do it soon, Scott will on his own.
Carol and Daniel were welcomed relief last night allowing Ashley and I to take a much needed break. Carol shared a couple humorous exchanges while in the ring. At one point Scott, as he often does, tried to get up out of bed. Carol asks Scott “Where are you going?” Scott looks at Carol with clear eyes and replies “On a Journey”. Carol then asked “Where is this journey taking you?” And Scott just sat back and mumbled the details at length of his imagined journey. On another exchange, Scott was aggressively kicking with his legs and Daniel asked Scott “What was going on?” “GOOOOOOOOAAAAAAAL!” was Scott’s response.
Ashley’s mom arrived just before Scott’s surgery and Patti will be here tomorrow morning. Carol and Daniel fly back to Dallas tonite. I will be heading back tomorrow and will look forward to returning April 11th. The guard changes again for the next phase of Scott’s recovery. I am caught reflecting what an unbelievable week this has been and how grateful we are for Scott’s rapid progress. We are truly blessed and are forever honored by your love and support.
Best!
Mickey Moore
Saturday, March 31, 2012
Friday, March 30, 2012
Day 17: Scott and Ashley Quality Time
Hello to all reading. It's Ashley.
Mickey covered todays happening really well. I wanted to share some of my perspective on today for just a minute. After the major insurance upset this morning, which left me in tears, I came back to Scott's room feeling frustrated and discouraged. I was really looking forward to moving on to the next stage of Scott's recovery. But despite all of that there were some very terrific things about today that brought a huge smile to my face.
1. While I was testing Scott's ability to read as well as see (by writing down words on a piece of paper) The first word I wrote was "Scott", the second word I wrote was "love", and the third word was "complicated." After Scott was able to read those words to me I asked him if he wanted to try writing a word. (The only problem is Scott is right handed so he tried writing by using his left.) I told him I would help him and I asked what word he wanted to write. The word he chose was "Joy" If that doesn't show you they type of guy Scott is I don't know what does.
2. Our CNA today was asked if she would give Scott a shave. She looked dumb struck and reluctant so I offered to help out and shave his face for her. I told her if she would bring me the stuff I would do it and it could save her some time. Now I really wish I had a video camera around because this process was definitely worth a laugh or two. Now I have never shaved a mans face before but I think I know my way around a razor and shaving cream. (I did have a "Shave Ken Barbie growing up... Yeah they actually make something like that) So off we set on this little experience together. Scott was set up in his wheel chair which made things a little easier. (I can't imagine if I were to try and shave him while he was in bed) It was a balancing act trying to make sure I didn't cut him, hurt him, or send any soapy water down his trach. Needless to say we got the job done and I he was patient with me the whole time. I only nicked him in a few places... sorry honey. But he looks more like my Scott now and I love it!!
3. After our shaving escapades I asked him if he wanted to drink some water. He made me laugh by asking the respiratory therapist to go get him a drink. With in a minute Scott had downed the water. I made sure that he was swallowing it all and not just choking on it. We refilled his cup 3 times.
4. Since he hadn't had any food since 12:00 the night before I asked him if he wanted to try to eat something. He said that he did. I asked if he wanted to have pudding or jello. He said he wanted pudding. So off I went to ask the nurses for some pudding. I successfully came back with some chocolate snack-pack pudding. We worked on him feeding himself. I was trying to encourage him to use his right hand to feed himself but it didn't work out so well. He took the pudding cup from me with his left hand and tried to drink it from the cup. This in turn caused him to have brown pudding all over his lips and nose. It made me laugh out loud. He then agreed to let me help him with his pudding.
5. Finally we were able to leave Select (fingers crossed that we don't have to go back there) we are now in St. Joseph's the main hospital. I can't begin to tell you all how much the staff here have impressed me. WOW. It is amazing to me how kind and considerate they have been.
6. Scott is becoming more and more capable of reasoning... except as to where his trach collar actually goes. He keeps insisting that it goes on his nose and his mouth. Every 10 seconds he has moved it back up and we have the conversation that it stays on his neck by his trach.
7. Tonight Scott told me that he wanted to go eat at Olive Garden. I told him that when he is feeling better we can for sure go eat there (or at least get some to go and bring it to rehab when he is able to eat solid food again)
8. When I asked Scott to calm down a little so that I could go eat my dinner he got really fidgety. He made every effort possible to get out of bed. I asked him if there was a reason he was trying to get out of bed and he replied. "I need to go get you dinner." Melted my heart. :)
9. Last night during one of our wrestling matches Scott said to me... "Your turn." Often times right before bed at night we will try and switch who says bed time prayer. To this one of us usually replies "your turn." I asked him if he wanted me to say our bedtime prayer and he said he did. I was able to hold his hand and say a little prayer of gratitude for our day and for all the progress he is making. We also wanted to thank our Heavenly Father for all the wonderful people who have shown love, prayers, and support through all of this. It was a sweet moment for me to share with him. I know he is grateful for all of you.
10. It really was a great day full of quality time with one another. It makes you stop and take a look at life and enjoy some of the smaller moments. Take a moment and enjoys some of those small moments with your families. Life is a precious gift that we sometimes forget the meaning of. Thank you all again for your continued concern, love, prayers, and support. I have truly felt lifted by all of it. We are holding strong and will continue to move forward.
Love you all,
Ashley
Day 17: Insurance Reform - Friday March 30, 2012
Last evening we got word that Scott’s facial surgery was scheduled for 1:00pm today. Hooray! He was off food and water as of midnight and we all sat, err... wrestled, excited through the night and morning as the next step toward getting to rehab was drawing near. We were told he would be picked up around 11:00am. Then at 10:30am we were told the surgery was canceled due to a problem with insurance.
We were told that the insurance company could not assign a required case number in time for the surgery because of the dynamics involving multiple lead surgeons and the complexity of the procedures. The case number was required only because the surgery was to be performed at St. Joseph’s but he was a patient of Select. We now have to admit Scott to St. Joseph’s first. Once admitted to St. Joseph's, Scott will not require the case number from the insurance and we will then proceed with surgery tomorrow (Saturday). Fortunately Scott should still be able to head to Barrows on Monday.
Warning - I personally take responsibility for all following editorial comments and apologize to those who work in the insurance industry that may take offense.
For many years there has been much political debate about healthcare reform. I believe the discussions should be about health insurance reform. The insurance “Middleman” is the real gatekeeper to health care and needs to be neutered. We the customer/patient should be able to act as consumers of healthcare, but instead we are subjects of corporate and statistical policy handed down by insurance companies. I encourage everyone to take control, do all you can to be a consumer to health care and not insurance. Yes, I believe that insurance as a catastrophic umbrella for protection is useful, however there is too much insurance sold as a means for people to be unaccountable. This is what I see as fundamentally wrong with insurance.
Sorry again for editorializing but Ashley and I were a bit peeved and I had to vent. Thanks for your indulgence.
Now back to Scott. His short term memory is not good and Ashley and I continue to work with him, asking questions of recent happenings. He is very much in the now and responds only to an immediate situation or stimulation. This is definitely adding to his agitated state when awake as the senses of feel take over. So much for reason helping us. Scott repeats what he hears a lot and when we need for him to tell us what he wants, we need to be clear that we do not suggest the answer.
We tried something else for the first time today. Ashley wrote words on a piece of paper and had him read them. He was able to with both eyes. (NOTE - this has since been shown not to be the case as he was later diagnosed with Marcus Gunn Pupil which most likely will result in the loss of eyesight in the right eye) His speech is getting clearer (even without the speaking valve) and we are beginning to understand some of his mumbled ramblings. Last night I swear he said he wanted to go fishing. He definitely said to me “I have a wonderful wife” as Ashley was leaving the room to go down the hall (Insert tear of joy emoticon here).
The Shoulder MRI results arrived. There is no nerve or soft tissue damage, only the grade 3 AC separation. This pretty much confirms that the lack of movement with that arm and the right leg is due to the brain injury. Barrow will for sure be working on that. Patti will be assisting with the ortho rehab of the shoulder as well.
Ashley and I are excited for Scott to have more family with him this weekend providing additional stimulation. Also for the additional tag-team partners.
Joy!
Mickey Moore
We were told that the insurance company could not assign a required case number in time for the surgery because of the dynamics involving multiple lead surgeons and the complexity of the procedures. The case number was required only because the surgery was to be performed at St. Joseph’s but he was a patient of Select. We now have to admit Scott to St. Joseph’s first. Once admitted to St. Joseph's, Scott will not require the case number from the insurance and we will then proceed with surgery tomorrow (Saturday). Fortunately Scott should still be able to head to Barrows on Monday.
Warning - I personally take responsibility for all following editorial comments and apologize to those who work in the insurance industry that may take offense.
For many years there has been much political debate about healthcare reform. I believe the discussions should be about health insurance reform. The insurance “Middleman” is the real gatekeeper to health care and needs to be neutered. We the customer/patient should be able to act as consumers of healthcare, but instead we are subjects of corporate and statistical policy handed down by insurance companies. I encourage everyone to take control, do all you can to be a consumer to health care and not insurance. Yes, I believe that insurance as a catastrophic umbrella for protection is useful, however there is too much insurance sold as a means for people to be unaccountable. This is what I see as fundamentally wrong with insurance.
Sorry again for editorializing but Ashley and I were a bit peeved and I had to vent. Thanks for your indulgence.
Now back to Scott. His short term memory is not good and Ashley and I continue to work with him, asking questions of recent happenings. He is very much in the now and responds only to an immediate situation or stimulation. This is definitely adding to his agitated state when awake as the senses of feel take over. So much for reason helping us. Scott repeats what he hears a lot and when we need for him to tell us what he wants, we need to be clear that we do not suggest the answer.
We tried something else for the first time today. Ashley wrote words on a piece of paper and had him read them. He was able to with both eyes. (NOTE - this has since been shown not to be the case as he was later diagnosed with Marcus Gunn Pupil which most likely will result in the loss of eyesight in the right eye) His speech is getting clearer (even without the speaking valve) and we are beginning to understand some of his mumbled ramblings. Last night I swear he said he wanted to go fishing. He definitely said to me “I have a wonderful wife” as Ashley was leaving the room to go down the hall (Insert tear of joy emoticon here).
The Shoulder MRI results arrived. There is no nerve or soft tissue damage, only the grade 3 AC separation. This pretty much confirms that the lack of movement with that arm and the right leg is due to the brain injury. Barrow will for sure be working on that. Patti will be assisting with the ortho rehab of the shoulder as well.
Ashley and I are excited for Scott to have more family with him this weekend providing additional stimulation. Also for the additional tag-team partners.
Joy!
Mickey Moore
Thursday, March 29, 2012
Day 16: Rehab Hear We Come!!!
Wow!!! The prayers are working!!! We thought Scott would be in ICU for 2 weeks and then in the LTAC facility for 2-3 weeks... and possibly 2 weeks in a Sub-acute setting before finally landing at Barrow Neurological Institute (BNI). Now it looks like it might be a day shy of 3 weeks (depending on the outcome and recovery of his surgery tomorrow) that he can transfer to BNI!!! Truly amazing and exciting! So... Thank you Thank you Thank you! for all of the many prayers, fasts, and temple work! We are extremely grateful! Scott has made greater than anticipated progress this week! We are beyond thrilled, and very hopeful. We know we have a long haul still ahead of us, but it is definitely uplifting to have a week like this one with a lot of progress.


We are definitely excited about transferring to Barrow. Barrow is a world-renowned facility. Representative Gabby Giffords went there, as well, following her gun-shot wound. The transfer to BNI means he is strong enough to tolerate 3 hours of therapy per day and alert enough to participate in 3 hours of therapy per day.
In some ways, we won't see as much progress as quickly. Medically, he is becoming so much more stable and less dependent on external support. Rehab progress tends to be slower. We all know how painfully long it takes when we are trying to get stronger or build endurance. It requires a lot of repetition and time to re-build what only took a matter of weeks to break down. Scott has lost 30 pounds already! Egads! We all know he had the absolute minimum of fat to begin with, so you can imagine that a lot of that weight loss is muscle atrophy.
Neurological healing is even slower, typically. Nerve tissue can regenerate if not too badly damaged, but the process is extremely slow. The rapid progress we have seen over the past 2 weeks is likely due to resolving swelling in the brain. Therefore, the lessened swelling is impairing his cognitive function less as the swelling dissipates. Any actual brain damage, will be slower to heal. We do expect his rate of progress to plateau at some point. So we won't always have the big, exciting, daily progress that we have had this week to report.
Being at Barrow will facilitate faster gains, for sure. Three hours of therapy per day definitely works! ... And we are all anxious to learn what we can do help. There will be roles for all of us in this process.
Barrow has a great educational document that they have prepared for patients and families. I am including the link for those who also have an interest. We actually recommend reading it for those who plan to visit Scott at Barrow. It will answer a lot of your questions and it will help prepare you, and allow you greater confidence in your interactions with Scott.
The most important section to read is the "Recovery after Brain Injury" section, pages 20-26. For the Reader's Digest version... Page 22 applies to Scott in his current condition.
http://www.thebarrow.org/stellent/groups/public/@xinternet_con_bni/documents/webcontent/bnp00046.pdf
Helpful information for those who do read the full document:
1. Scott had Diffuse Axonal Injury (DAI), grade II, and a right temporal epidural hematoma.
2. He did not have any secondary injuries (cerebral anoxia/hypoxia, increased intracranial pressure, or seizure) that we are aware of. He has been on anti-seizure medication since the accident, however, due to the high risk of seizures with DAI. He will be at increased risk for seizures for 2 years.
3. He is no longer considered to be in a coma. His original Glasgow Coma Scale score was 7. It is now 15.
4. The Rancho Los Amigos Scale will be the best scale at this point in his recovery to measure his status and progress. Originally, he scored a II. Now he would score a IV or a V ...hard for me to discern for sure until I can see him in person on Sunday. I am thrilled how quickly he has moved up these scales. I thought the progress on this scale would be slower, for sure.
5. He is considered to have had a severe brain injury.
6. Medical Management:
a) He does have various other injuries and fractures to manage.
b) Again, we are on the watchout for seizures.
c) Scott has had significant high blood pressure and tachycardia (Fast heart rate)in response to his head injury.
d) Heterotrophic Ossification (HO) - We won't know about for quite some time if he will suffer this side-effect. This is the weirdest possible complication, in my mind. I am extremely interested in finding out more about the how's and why's of this. Basically, for those who don't read the document, abnormal bone growth can occur in joints, in places that bone should not be, following a TBI (traumatic brain injury). It is most common in the shoulders and hips. Simply crazy to me! If anyone out there knows why HO occurs following TBI (I want to know the physiology behind it), please let me know!

Good involvement of family and friends is stated (in the BNI document) to positively impact the outcome of TBI patients. This is where we will begin to need help. We have been instructed/counseled to provide stimulation for Scott (one stimulation at a time, brief sessions (i.e., 1-2 minutes at this point) and to vary the stimulation to effect all 5 senses).
Once Scott transfers to Barrow, he should be strong enough to have visitors. We know that a lot of family and friends have been anxiously awaiting this day, when they can come to visit. We will need to schedule the visits to avoid overstimulating him and exhausting him, but we know he will love having visitors. We can see that there may be days when someone is scheduled to visit, and we may need to call to say "not today". Just want everyone to have a heads up on that.
I (Patti) will coordinate the visitation schedule. If you are interested in visiting Scott, you may reach me at 801-589-1466 or pjdn150@gmail.com. You are more than welcome to simply visit....The social stimulation will be fun for Scott and will be stimulating to him, for sure. ...But... If you would like to bring an idea or a prop to provide brief (1-2 minutes) stimulation for one of the 5 senses (sight, hearing, smell, taste, touch), that would be a bonus! A short, simple game could even be a good option. I am sure he will get much more variety this way, which will be more fun as well as more challenging and stimulating to him!
Also, for those with the ability to make a short (1-2 minutes) video.... you may video a message for Scott, email it to me at pjdn150@gmail.com, and we will play it for Scott when he is alert and awake.
We are excited for this next stage! Surgery tomorrow.... post-op recovery for a few days, ... then off to Barrow!
Love to all!
Patti


We are definitely excited about transferring to Barrow. Barrow is a world-renowned facility. Representative Gabby Giffords went there, as well, following her gun-shot wound. The transfer to BNI means he is strong enough to tolerate 3 hours of therapy per day and alert enough to participate in 3 hours of therapy per day.
In some ways, we won't see as much progress as quickly. Medically, he is becoming so much more stable and less dependent on external support. Rehab progress tends to be slower. We all know how painfully long it takes when we are trying to get stronger or build endurance. It requires a lot of repetition and time to re-build what only took a matter of weeks to break down. Scott has lost 30 pounds already! Egads! We all know he had the absolute minimum of fat to begin with, so you can imagine that a lot of that weight loss is muscle atrophy.
Neurological healing is even slower, typically. Nerve tissue can regenerate if not too badly damaged, but the process is extremely slow. The rapid progress we have seen over the past 2 weeks is likely due to resolving swelling in the brain. Therefore, the lessened swelling is impairing his cognitive function less as the swelling dissipates. Any actual brain damage, will be slower to heal. We do expect his rate of progress to plateau at some point. So we won't always have the big, exciting, daily progress that we have had this week to report.
Being at Barrow will facilitate faster gains, for sure. Three hours of therapy per day definitely works! ... And we are all anxious to learn what we can do help. There will be roles for all of us in this process.
Barrow has a great educational document that they have prepared for patients and families. I am including the link for those who also have an interest. We actually recommend reading it for those who plan to visit Scott at Barrow. It will answer a lot of your questions and it will help prepare you, and allow you greater confidence in your interactions with Scott.
The most important section to read is the "Recovery after Brain Injury" section, pages 20-26. For the Reader's Digest version... Page 22 applies to Scott in his current condition.
http://www.thebarrow.org/stellent/groups/public/@xinternet_con_bni/documents/webcontent/bnp00046.pdf
Helpful information for those who do read the full document:
1. Scott had Diffuse Axonal Injury (DAI), grade II, and a right temporal epidural hematoma.
2. He did not have any secondary injuries (cerebral anoxia/hypoxia, increased intracranial pressure, or seizure) that we are aware of. He has been on anti-seizure medication since the accident, however, due to the high risk of seizures with DAI. He will be at increased risk for seizures for 2 years.
3. He is no longer considered to be in a coma. His original Glasgow Coma Scale score was 7. It is now 15.
4. The Rancho Los Amigos Scale will be the best scale at this point in his recovery to measure his status and progress. Originally, he scored a II. Now he would score a IV or a V ...hard for me to discern for sure until I can see him in person on Sunday. I am thrilled how quickly he has moved up these scales. I thought the progress on this scale would be slower, for sure.
5. He is considered to have had a severe brain injury.
6. Medical Management:
a) He does have various other injuries and fractures to manage.
b) Again, we are on the watchout for seizures.
c) Scott has had significant high blood pressure and tachycardia (Fast heart rate)in response to his head injury.
d) Heterotrophic Ossification (HO) - We won't know about for quite some time if he will suffer this side-effect. This is the weirdest possible complication, in my mind. I am extremely interested in finding out more about the how's and why's of this. Basically, for those who don't read the document, abnormal bone growth can occur in joints, in places that bone should not be, following a TBI (traumatic brain injury). It is most common in the shoulders and hips. Simply crazy to me! If anyone out there knows why HO occurs following TBI (I want to know the physiology behind it), please let me know!

Good involvement of family and friends is stated (in the BNI document) to positively impact the outcome of TBI patients. This is where we will begin to need help. We have been instructed/counseled to provide stimulation for Scott (one stimulation at a time, brief sessions (i.e., 1-2 minutes at this point) and to vary the stimulation to effect all 5 senses).
Once Scott transfers to Barrow, he should be strong enough to have visitors. We know that a lot of family and friends have been anxiously awaiting this day, when they can come to visit. We will need to schedule the visits to avoid overstimulating him and exhausting him, but we know he will love having visitors. We can see that there may be days when someone is scheduled to visit, and we may need to call to say "not today". Just want everyone to have a heads up on that.
I (Patti) will coordinate the visitation schedule. If you are interested in visiting Scott, you may reach me at 801-589-1466 or pjdn150@gmail.com. You are more than welcome to simply visit....The social stimulation will be fun for Scott and will be stimulating to him, for sure. ...But... If you would like to bring an idea or a prop to provide brief (1-2 minutes) stimulation for one of the 5 senses (sight, hearing, smell, taste, touch), that would be a bonus! A short, simple game could even be a good option. I am sure he will get much more variety this way, which will be more fun as well as more challenging and stimulating to him!
Also, for those with the ability to make a short (1-2 minutes) video.... you may video a message for Scott, email it to me at pjdn150@gmail.com, and we will play it for Scott when he is alert and awake.
We are excited for this next stage! Surgery tomorrow.... post-op recovery for a few days, ... then off to Barrow!
Love to all!
Patti
Day 16: Our Stay at Long-Term Care Ends Soon! - Thursday March 29, 2012
Last evening we had the Barrow Neurological Institute consult and they want to admit Scott after his facial surgery, probably Monday if his surgery is Friday. This is huge as he will immediately jump from a Long-Term Care Hospital to Rehabilitation. The Barrow Consulting Physician said that Scott meets all required criteria and that a couple of his classmates are actually doing their clinical rotations there at this time. They are very excited to help him heal. This news has added to the smile on Ashley’s face.
We all know that Scott is special, but being able to speak with a trach, without a speaking valve in place, had not been witnessed by the nursing staff. But there he was through the night, able to speak without it. When the Pulmonary Physician came by this morning he said that the trach would be coming out if it weren't for the surgery. The Respiratory Therapist then gave Scott some Jello to eat. He even took the spoon and fed himself a little. So now he can eat pureed foods. The Jaw will still require a week to mend before actual chewing is allowed.
The other thing Scott learned through the night was to use his mouth to remove the pillow mits covering his hands that keep him from pulling his trach out. Wrestlemania continues...
My post yesterday mentioned that Scott had his Shoulder MRI yesterday afternoon. Well he went and decided to wrestle with the MRI technicians. Why should Ashley and I have all the fun? Because he could not stay still, the MRI was rescheduled for this morning with a sedated Scott. This left Scott a bit out of it through the morning. Although groggy, it did not keep him from wanting to be in the wheelchair. Eventually we even took a stroll outside.
The facial surgery has yet to be scheduled so it will most likely not happen today. We sure hope they can get all the physicians together and schedule it for Friday. This now appears to be our last step before heading to Rehab!
Ashley’s mom is arriving on Saturday for a week and Carol and Step Brother Daniel for the weekend. Patti and I will be swapping duties this Sunday which is perfect timing for her to guide the transition to rehabilitation. Scott wouldn’t have it any other way.
Joy!
Mickey Moore
We all know that Scott is special, but being able to speak with a trach, without a speaking valve in place, had not been witnessed by the nursing staff. But there he was through the night, able to speak without it. When the Pulmonary Physician came by this morning he said that the trach would be coming out if it weren't for the surgery. The Respiratory Therapist then gave Scott some Jello to eat. He even took the spoon and fed himself a little. So now he can eat pureed foods. The Jaw will still require a week to mend before actual chewing is allowed.
The other thing Scott learned through the night was to use his mouth to remove the pillow mits covering his hands that keep him from pulling his trach out. Wrestlemania continues...
My post yesterday mentioned that Scott had his Shoulder MRI yesterday afternoon. Well he went and decided to wrestle with the MRI technicians. Why should Ashley and I have all the fun? Because he could not stay still, the MRI was rescheduled for this morning with a sedated Scott. This left Scott a bit out of it through the morning. Although groggy, it did not keep him from wanting to be in the wheelchair. Eventually we even took a stroll outside.
The facial surgery has yet to be scheduled so it will most likely not happen today. We sure hope they can get all the physicians together and schedule it for Friday. This now appears to be our last step before heading to Rehab!
Ashley’s mom is arriving on Saturday for a week and Carol and Step Brother Daniel for the weekend. Patti and I will be swapping duties this Sunday which is perfect timing for her to guide the transition to rehabilitation. Scott wouldn’t have it any other way.
Joy!
Mickey Moore
Wednesday, March 28, 2012
Day 15: Two Steps Forward, One Step Back - Wednesday March 28, 2012
Last evening the results from the facial CAT Scan arrived. Scott will need major facial surgery to repair sinus cavities that have been compromised and lower right eye socket and cheek reconstruction. This will be done this week, either Thursday or Friday. The sinus cavities are of significant concern as when compromised or blocked can harbor bacteria that can infect the brain. This is the reason for the quick surgical response. In addition a neurological physician from Barrow will be in on the surgery. The good news... Ashley and I were about to shave him but we’ll now probably let the surgical prep work their magic.
Due to the surgery the Pulmonary Physician said he will leave the larger trach in until after the surgery. This hasn’t seemed to stop Scott from speaking stronger today and drinking a cup and a half of water, one small sip at a time. A number of mental, memory and reasoning questions were posed. He passed all with flying colors. Here is a sample of what was asked:
Q) What year is it? - A) Two thousand twelve
Q) What city do you live in? - A) Glendale
Q) Do you know why you are here? - A) No
Q) Do you want me to tell you why? - A)Yes - Ashley then told Scott about the accident
Q) Can you float a leaf on water? - A) Yes
Q) Are there fish in the sea? - A) Yes
Q) Which is heavier, one pound or two pounds? - A) Two pounds
Q) What kind of Doctor will I become (Asked by friend Nate) - A) A Good One
Then the real tricky one...
Q) Die fenster or der fenster? - A) Das fenster
For those who do not speak German this question asked for him to identify the gender of fenster (German for window).
The Nurse also gave him a bit of a concentration test. She asked Scott to squeeze her hand every time she said the word “A”. She then went through a dozen or so random series of letter words including about six “A” words. Scott squeezed her hand for every “A” and did not for any others. This went on for about two minutes.
Morning PT today had Scott standing again, even straighter. He is able to briefly hold his head up on his own. We then sat him in a wheelchair and went for a ride out of the room! He interacted and got his bearings.
By late morning Scott was reasoning and understanding his situation, where he was and why certain things were attached to him. Now we have the upperhand managing his anxiousness and hyperactivity. We’ll just have to reorient him every time he wakes up as most likely current memory retention is not 100%.
This afternoon Scott finally had his MRI of the right Shoulder. Again they will be looking specifically for any possible nerve damage. We should have the MRI results in the morning and are still anxiously waiting for the Barrows Consult.
Scott has been able to keep the speaking valve in continuously. Another touching day with reasoned interaction by Scott continues to fuel everyone. We are so very blessed by your outpouring of love and for Scott’s improvement.
Mickey Moore
Due to the surgery the Pulmonary Physician said he will leave the larger trach in until after the surgery. This hasn’t seemed to stop Scott from speaking stronger today and drinking a cup and a half of water, one small sip at a time. A number of mental, memory and reasoning questions were posed. He passed all with flying colors. Here is a sample of what was asked:
Q) What year is it? - A) Two thousand twelve
Q) What city do you live in? - A) Glendale
Q) Do you know why you are here? - A) No
Q) Do you want me to tell you why? - A)Yes - Ashley then told Scott about the accident
Q) Can you float a leaf on water? - A) Yes
Q) Are there fish in the sea? - A) Yes
Q) Which is heavier, one pound or two pounds? - A) Two pounds
Q) What kind of Doctor will I become (Asked by friend Nate) - A) A Good One
Then the real tricky one...
Q) Die fenster or der fenster? - A) Das fenster
For those who do not speak German this question asked for him to identify the gender of fenster (German for window).
The Nurse also gave him a bit of a concentration test. She asked Scott to squeeze her hand every time she said the word “A”. She then went through a dozen or so random series of letter words including about six “A” words. Scott squeezed her hand for every “A” and did not for any others. This went on for about two minutes.
Morning PT today had Scott standing again, even straighter. He is able to briefly hold his head up on his own. We then sat him in a wheelchair and went for a ride out of the room! He interacted and got his bearings.
By late morning Scott was reasoning and understanding his situation, where he was and why certain things were attached to him. Now we have the upperhand managing his anxiousness and hyperactivity. We’ll just have to reorient him every time he wakes up as most likely current memory retention is not 100%.
This afternoon Scott finally had his MRI of the right Shoulder. Again they will be looking specifically for any possible nerve damage. We should have the MRI results in the morning and are still anxiously waiting for the Barrows Consult.
Scott has been able to keep the speaking valve in continuously. Another touching day with reasoned interaction by Scott continues to fuel everyone. We are so very blessed by your outpouring of love and for Scott’s improvement.
Mickey Moore
Tuesday, March 27, 2012
The rest of Day 14: Dreams Come True -, Tuesday March 27, 2012
For every parent, having a child become disconnected from your life as a result of tragedy or conflict, creates dreams of being re-united. Today, Scott has been able to express a reconnection with himself and with his family. This was especially moving as he and Ashley embraced and kissed through the afternoon. Embellished when he interacted with and thanked his sister Annie and her two children Myla and Tyce during a Skype video call. And punctuated as he wished me a “Good Nite”, reached out to bring me near and gave me a kiss on the cheek. I feel I can express that for all of Scott’s parents, Patti, Todd, Carol and myself, our dreams have come true today.
There were more medical advances this afternoon to share. Physical Therapy came and had Scott stand up three times. Each time he was able to stand assisted and straighten his back and head with help. See Photos:


Also during PT the Ortho consult came with the results of his shoulder x-rays. Everything was in the correct position so the next step is an MRI to look at the soft tissue, in particular the bundle of nerves along the shoulder. His lack of ability to move the right shoulder and arm may be caused by damage to those nerves. This would also require neurological treatments. The one thing the x-rays did confirm was a definite AC separation which is the cause of the lump on his shoulder. The PA valued it as a 2 to 3, I assume this is the grade of separation. Ashley and I have been working on the right arm and hand to reduce the stiffness and he is now holding it more loosely and using the elbow for stability more often.
I will close by sharing another conversation I had with Scott this afternoon. I asked Scott if he was in pain. Scott said “NO”. Then Scott said without prompting...”SHOULD I BE?”
Scott the Physician in training emerges!
Joy!
Mickey Moore
Day 14: Big Milestone - Tuesday March 27, 2012
SCOTT SPEAKS!!
An uplifting milestone this morning. After three hours in the ring with Scott, I had the nurses put him in the Med-Chair at around 7am for a change of environment. When the Pulmonary Physician came in he had the Respiratory Technician put the “Speaking Valve” on Scott’s trach. We had told him that Scott appeared to be mouthing words the past day. He then asked Scott “Do you know your name? “SCOTT MOORE” was Scott’s reply, clear as day! The physician said to use the speaking valve as much as Scott wanted.
We then recorded him saying “HI MOM”. (We are currently working on uploading that audio file). Then Ashley asked him “Do you know who I am?” And Scott said “MY WIFE”. Big grins ran amok throughout the entire floor.
When the Speech Therapist came she asked Scott if he wanted some water. Scott said yes and the following video shows Scott taking his first sips of water and swallowing. Sorry we weren't able to get it rotated.
Medically Scott had his Shoulder x-rays taken yesterday evening and a CAT Scan of his facial fractures taken this morning. Results of each should be forthcoming later today.
A great start to a beautiful day!
Mickey Moore
An uplifting milestone this morning. After three hours in the ring with Scott, I had the nurses put him in the Med-Chair at around 7am for a change of environment. When the Pulmonary Physician came in he had the Respiratory Technician put the “Speaking Valve” on Scott’s trach. We had told him that Scott appeared to be mouthing words the past day. He then asked Scott “Do you know your name? “SCOTT MOORE” was Scott’s reply, clear as day! The physician said to use the speaking valve as much as Scott wanted.
We then recorded him saying “HI MOM”. (We are currently working on uploading that audio file). Then Ashley asked him “Do you know who I am?” And Scott said “MY WIFE”. Big grins ran amok throughout the entire floor.
When the Speech Therapist came she asked Scott if he wanted some water. Scott said yes and the following video shows Scott taking his first sips of water and swallowing. Sorry we weren't able to get it rotated.
Medically Scott had his Shoulder x-rays taken yesterday evening and a CAT Scan of his facial fractures taken this morning. Results of each should be forthcoming later today.
A great start to a beautiful day!
Mickey Moore
Day 13/14: Wrestlemania & Sleep Depravation
Poor Scott. Tonight has been one long wrestling match after another. We waited till 10 pm to give him any medication so that he might sleep better through the night. It took about a half hour of me wrestling him into bed and then he had a bowel movement. After that I hoped he would calm down. Eventually the medication kicked in. We both got a few hours of sleep until Scott tried to pull a Houdini on me and escape his roll belt, side pads, and railing. He managed to make it half way off the bed pulling off his oxygen tube, condom catheter and the attachment to his feeding tube. When I finally woke up to all the commotion I was worried that he might have pulled his feeding tube out of his stomach, thankfully that wasn't the case.
Scott starts with the left leg and moves it over the the side padding. He then uses that left leg to pull himself closer to the edge of the bed. He is able to use the right leg more so he skillfully places that over the edge of the bed as well. He then uses his left elbow to start sitting up as much as possible. Often times he will grab at the side rails to pull himself to whatever side he prefers. (The roll belt basically wraps around his torso and ties on opposite sides of the bed. This helps keep him from sitting all the way up, or falling all the way out of bed.)
If I can catch him before both legs are over the edge of the bed I can usually lift his legs up and pull them back around into bed. Sometimes when I am sitting next to the bed he will use me as his leverage to pull himself up. I have almost ended up in the bed with him a few times. I forget how strong he is.
After this last incident they decided that he would need to have mitts put on. They basically look like small pillow boxing gloves that tie at the wrist of the hand. He hates them and it makes me feel like a terrible person for having to do this to him. I just have to remind myself that it's to keep him safe.
I don't feel like I can go to sleep because each time I do he ends up almost on the floor or ripping something off. I was joking with the nurses that this situation reminds me of a new mom and baby. You're tired and sleep deprived and want your baby to go to sleep but the moment the baby is asleep and you wake up and they aren't crying you immediately worry that something is wrong. That is why I am sitting up writing this post at 4 am... He is finally starting to calm down enough (thanks to a recent dose of Meds) that I don't have to wrestle him, but I do need to keep my eyes on him.
Thankfully Mickey should be here soon to tag in so I can get some sleep.
Good Night or Morning to you all,
Love Ashley
Monday, March 26, 2012
Day 13: Relentless Energy - Monday March 26, 2012
WOW - Scott was relentless through the night, rolling side to side, throwing his legs and hips out of bed, trying to sit up and self doctoring himself by removing tubes. Eventually the nurses had to use a roll strap to keep him in the bed.
Morning temp and BP are normal. Pulmonary Physician says everything sounds great. He didn’t say specifically when the trach would be exchanged for a smaller one, just “sometime this week”.
Wound Care has been amazed at the rate of Scott’s skin regeneration. The road rash on his right arm is fully healed and the only wound requiring wrapping today was the friction burn on his left arm. This is good as the wraps don’t last very long when he is so active. The surgery incision on his right arm is open to the air and about half of the staples are “floating” which means they are close to needing to be removed. Today’s big removal was the remaining staples in his head.
Physical Therapy was in and put Scott sitting on the side of his bed while they helped him attempt to hold his head and back straight up and down. He did amazing responding to commands but could not straighten on his own. Afterward he sat in the Med-Chair for three hours.
Scott’s Attending Physician is now organizing the other specialists that Scott will need including Ortho, Barrow and Ophthalmology. Ortho dropped by in the afternoon and the initial evaluation is an AC separation with possible dislocation. X-Rays have been ordered and we are waiting for that to happen. We are also waiting for the Barrow Consult as our ultimate goal is to get Scott to that facility when appropriate.
A very encouraging moment came during the Ortho Consult. I had called Patti to have her listen into the exam and put the phone to Scott’s ear so she could say hello. Upon hearing her voice he immediately opened his mouth and appeared to try to say “Hi”. Of course with the current trach he cannot make any noise but we sure feel he will be ready for the speaking trach later this week.
Fortunately or unfortunately Scott has been much calmer during the day today than last night. His pulse has been a bit more elevated than yesterday and they are keeping him on pain medication which helps calm him. We fear though that we are helping to mix up his days and nights. I’m sure he will cycle back and forth more than once.
Each of the last three days I am seeing more brightness and spark in his eyes. Awareness is certainly improving and often I speak to him as if he just woke up for the first time, telling him he was in an accident and getting better in the hospital. This morning it struck me that this recovery process is similar to his infant years and early development childhood. He was not an easy infant so why should we expect this stage of his recovery to be any different. No matter, Scott’s return is worth much more.
Blessings to all
Mickey Moore
Morning temp and BP are normal. Pulmonary Physician says everything sounds great. He didn’t say specifically when the trach would be exchanged for a smaller one, just “sometime this week”.
Wound Care has been amazed at the rate of Scott’s skin regeneration. The road rash on his right arm is fully healed and the only wound requiring wrapping today was the friction burn on his left arm. This is good as the wraps don’t last very long when he is so active. The surgery incision on his right arm is open to the air and about half of the staples are “floating” which means they are close to needing to be removed. Today’s big removal was the remaining staples in his head.
Physical Therapy was in and put Scott sitting on the side of his bed while they helped him attempt to hold his head and back straight up and down. He did amazing responding to commands but could not straighten on his own. Afterward he sat in the Med-Chair for three hours.
Scott’s Attending Physician is now organizing the other specialists that Scott will need including Ortho, Barrow and Ophthalmology. Ortho dropped by in the afternoon and the initial evaluation is an AC separation with possible dislocation. X-Rays have been ordered and we are waiting for that to happen. We are also waiting for the Barrow Consult as our ultimate goal is to get Scott to that facility when appropriate.
A very encouraging moment came during the Ortho Consult. I had called Patti to have her listen into the exam and put the phone to Scott’s ear so she could say hello. Upon hearing her voice he immediately opened his mouth and appeared to try to say “Hi”. Of course with the current trach he cannot make any noise but we sure feel he will be ready for the speaking trach later this week.
Fortunately or unfortunately Scott has been much calmer during the day today than last night. His pulse has been a bit more elevated than yesterday and they are keeping him on pain medication which helps calm him. We fear though that we are helping to mix up his days and nights. I’m sure he will cycle back and forth more than once.
Each of the last three days I am seeing more brightness and spark in his eyes. Awareness is certainly improving and often I speak to him as if he just woke up for the first time, telling him he was in an accident and getting better in the hospital. This morning it struck me that this recovery process is similar to his infant years and early development childhood. He was not an easy infant so why should we expect this stage of his recovery to be any different. No matter, Scott’s return is worth much more.
Blessings to all
Mickey Moore
Day 13: Hope and Positivity- March 26, 2012
A few words that come to mind when I think of Scott are:
Positive
Intelligent
Loving
Driven
Energetic
Happy
Service Oriented
I wanted to take a moment today and post a few photos of Scott that reflect those words. I know that Scott would want us to remain positive during this time.
So I hope these photos bring a smile to your face.
Keep up your hope, prayers, and positivity!!
We love you ALL!
 |
| October 2011 |
 |
| City of Rocks- June 2009 |
 |
| Echo Triathlon July 2008 |
 |
| Phoenix Coyotes Hockey Game - December 2011 |
 |
| Scott playing his guitar during the USA- Pro Cycling Challenge in Colorado (August 2011) |
 |
| Scott and Ashley after church January 2012 |
 |
| Our Silly Valentine's Day photos. Having some fun with mustaches. Feb 14, 2012 |
 |
| Boston Marathon April 2010 |
 |
Scott doing Clinical Laboratory research on DePEGylation of Blood Cells.
(Later published in the Magazine of Clinical Laboratory Science. On September 22, 2011)
|
 |
| Scott in his Air Force Uniform after C.O.T. June 2009 |
 |
| Scott and Ashley Salt Lake City Temple May 2011 |
 |
| Scott at Commissioned Officer Training June 2009 |
 |
| Scott and Ashley building decks in Oregon. Alternative Spring Break - Habitat For Humanity March - 2008 |
 |
| Antelope Island Buffalo Duathlon - May 2008 |
Sunday, March 25, 2012
Day 12: Bazinga - Sunday March 25, 2012
Scott had a very restful night. They gave him Seroquel in the evening and it really calmed him down. The nursing response was much better and Ashley was able to rest. Perhaps we also wore Scott out during the day yesterday and have avoided him switching days and nights. We can only hope.

Half of the staples securing the incision in Scott’s head were removed today. The other half will be removed in a couple days.
This afternoon we Skyped Ryan Moore, Scott’s brother in Dallas and the two had a video conference call. Scott definitely reacted to Ryan’s voice and kept his eyes open and on the monitor the whole time.
This afternoon Scott has been very active. We did give him some Tylenol thinking it would calm him as it did the previous day but no such luck. We’re letting him go so he doesn’t get his days and nights confused. He is being quite a handfull and actually seems to be trying to get out of the bed.
Ashley was able to go out with her friends for awhile and enjoy dinner and a shower at home. We’ll take any break for her that we can get.
Overall the day has been very active without any significant change in awareness. We hope he rests well tonight as he did last night so Ashley can get some sleep.
Humorous mental picture of the day: Ashley singing “Soft Kitty” to Scott. BAZINGA!
 Soft Kitty Image by Petit-J (deviantart.com) |
- Mickey Moore
Saturday, March 24, 2012
Day 11: Changing of the Guard Part 2
I am writing this as I sit on a plane headed for Salt Lake City. It feels so wrong. It just feels too early for a mother to leave her son in this situation. Arguably one of the hardest things I have had to do in my life! It was a committee decision and logically, it makes sense, but emotionally...not so much! As a support team, we decided to take shifts, since this will be a long and arduous road ahead....Pacing is a very smart idea. So... Michael, Scott's dad, is there with Ashley this week. The good news about being gone for 5 days is that he will likely have made some big improvements when I get back. He will have his speaking valve in, and he may be eating and talking.
The blog reigns will be handed over while I am in Utah. I will be as anxious for posts as the rest of you!
Last night, Scott was very active. We have been told that he will become more active as he becomes more awake. The tough piece is knowing when the restlessness is due to pain (bad) and when it is due to increased consciousness (good). His pulse rate has been our indicator, so far. His pulse rate is commonly 120-130 when he is in pain, but remains in the 70's and 80's when he is "just awake". He did get quite aggressive at tugging on things last night, though. He pulled out his IV, his trach canula (the inner tubing), his catheter, and his pulse oximeter. He gave the night crew a run for their money. He also did a gazillion partial sit ups in bed last night, and is now rolling over onto his sides by himself...both sides/even the right! He is visually tracking to sounds, at times. They will put a smaller trach tube in on Monday... the speaking valve will be next....then maybe eating (if he is more awake). They have taken the ventilator out of the room, since he has gone 3 days and nights without needing it. Yeah!
We have been tapping into our family resources this week to help us understand and manage this phase of Scott's recovery. It has been a huge learning curve for us. My fabulous sister-in-law, Robin, who is an RN, has a lot of experience in critical care, teaches nursing students, and has been a legal consultant for medical malpractice cases for many many years has been an extremely valuable resource for us in adjusting to the LTAC phase. Thank you so very much, Robin!
She also has a contact that she has used as an expert witness in the past, who was a neurosurgeon at Barrows for many years. She contacted him re: general Barrows Neurological Institute qualilfication questions that we had. In their discussion, he said that it was GREAT (his words and his emphasis) that Scottie has been able to follow commands before the 2 week mark... It will be a long road, but there is hope. It seems like such a long way away right now as he vacantly stares past us when we look at him and talk to him.... when he can't even hold his head up or stick out his tongue,....but it is reassuring to know that time is on our side and will be our friend in this case!

Keep the prayers coming... I'll "talk" to you again in a few days... for now, Ashley and Michael will be at the blog helm!
Love you all!
- Patti
Day 11: Changing of the Guard, Saturday March 24, 2012
This is Mickey Moore signing in with today’s report. Patti flew back to Utah this afternoon and I’ll be doing my best to support Ashley and Scott through the upcoming week. Patti’s support has been not only a tremendous value but has taken a tremendous effort, and we hope she is able to re-charge. Going forward, Patti’s and my intent will be to take turns here in Phoenix a week or so at a time.
Scott had a very restless night and successfully removed the IV from his hand and the inner sleeve from his trach. There were some issues with the response time during the night by the nurses and Patti and Ashley have since had a conversation with the Charge Nurse to “clear the air”. It was good to know that our expectations, which were not met, were reasonable and an escalation path determined. It was also very helpful to have input from Robin Doctor who offered great context of our situation. Once again communication is key.
One major outcome of this last meeting is that we now have a list of all prescribed medications, both scheduled and as-needed. This way we can double-check with the nurses when they are administering the drugs. Although the nurses have been very good about telling us what they are giving him, we have had no reference as to whether it was ordered. Now we do.
Patti and Ashley have been sleeping in Scott’s room every night and for now Ashley will continue to do so. I have been able to leave for the night and each time I return some 12 hours later, Scott shows marked improvement. I’ve mentioned to Ashley that she should also try sleeping at home just to see the change in 12 hours (nudge... nudge...) in the hope that she will find her own path to maintaining her level of health and energy. I feel certain that just like Scott, Ashley knows when the time is right.
This morning Scott sat in the med-chair for over two and a half hours. He tired a bit and slumped down often but would help me on command to scoot back upright. He worked very hard the entire time. PT will be amazed on Monday if he keeps this up.
Scott is rolling onto both sides when active and beginning to recognize changes in his surroundings. The day Respiratory Technician came in the room when Scott was sitting up and Scott immediately turned his head and opened both eyes at the Tech.
This afternoon he was so active and tired (all Moore boy’s ears turn bright red when tired) that we had the nurse give him a little tylenol and he went right to sleep. I’m no expert but I swear that I saw evidence of deep REM sleep when his right eyelid began to flutter. I hope that is a sign of additional neural activity that we have not seen to date.
One definite good sign is that he is urinating on his own without catheterization. This is significant as his neurological system regains control of all bodily functions.
Ashley and I anticipate a very active and progressive week. Scott will be a handful as he continues to gain more awareness. We will do our best to provide a day-by day, blow-by-blow account through this week.
Carol and I thank everyone for all the thoughts and prayers. We have just begun to support Scott’s challenge and are fueled by your love.
Mickey Moore
Scott had a very restless night and successfully removed the IV from his hand and the inner sleeve from his trach. There were some issues with the response time during the night by the nurses and Patti and Ashley have since had a conversation with the Charge Nurse to “clear the air”. It was good to know that our expectations, which were not met, were reasonable and an escalation path determined. It was also very helpful to have input from Robin Doctor who offered great context of our situation. Once again communication is key.
One major outcome of this last meeting is that we now have a list of all prescribed medications, both scheduled and as-needed. This way we can double-check with the nurses when they are administering the drugs. Although the nurses have been very good about telling us what they are giving him, we have had no reference as to whether it was ordered. Now we do.
Patti and Ashley have been sleeping in Scott’s room every night and for now Ashley will continue to do so. I have been able to leave for the night and each time I return some 12 hours later, Scott shows marked improvement. I’ve mentioned to Ashley that she should also try sleeping at home just to see the change in 12 hours (nudge... nudge...) in the hope that she will find her own path to maintaining her level of health and energy. I feel certain that just like Scott, Ashley knows when the time is right.
This morning Scott sat in the med-chair for over two and a half hours. He tired a bit and slumped down often but would help me on command to scoot back upright. He worked very hard the entire time. PT will be amazed on Monday if he keeps this up.
Scott is rolling onto both sides when active and beginning to recognize changes in his surroundings. The day Respiratory Technician came in the room when Scott was sitting up and Scott immediately turned his head and opened both eyes at the Tech.
This afternoon he was so active and tired (all Moore boy’s ears turn bright red when tired) that we had the nurse give him a little tylenol and he went right to sleep. I’m no expert but I swear that I saw evidence of deep REM sleep when his right eyelid began to flutter. I hope that is a sign of additional neural activity that we have not seen to date.
One definite good sign is that he is urinating on his own without catheterization. This is significant as his neurological system regains control of all bodily functions.
Ashley and I anticipate a very active and progressive week. Scott will be a handful as he continues to gain more awareness. We will do our best to provide a day-by day, blow-by-blow account through this week.
Carol and I thank everyone for all the thoughts and prayers. We have just begun to support Scott’s challenge and are fueled by your love.
Mickey Moore
Friday, March 23, 2012
Day 10: A better day today. March 23, 2012
We are glad to report that today is a better day. The team has responded promptly and well to our concerns. Communication has improved and we see active problem solving for his "issues". We have a better grasp of what to expect and a better sense that they are acting in a pro-active manner.
The nurse last night, took good care of him. His pulse rate has been really high, generally 100 to 113. We have been told that it would be expected, but it is hard to see as a constant, knowing that his normal pulse rate is 56. And... I don't know if it is due to pain, due to neuro issues, etc. he nurse last night did some problem solving, which we appreciated. She asked him through hand squeezes if he was in pain, further assessed the accuracy of his responses and reliability of his responses. She gave him a some pain meds, then his pulse rate decreased to 78 from 120 plus. So I guess we have our answer. I can only imagine that he has a ton of pain with all of his fractures, surgeries, and head trauma. The trick is making him comfortable at night so he can rest and recover, but not over medicating him so he can't participate with therapies during the day or progress his awareness. Such a trick. It would really help to Assess him and help him if he was awake!
A different doc came in today. We liked him much better. Much more pro- active, much better communicator. We are glad to have him for the weekend. We asked to have him routinely. Not sure that will happen, though. He did say that he would like to have Physiatrist from Barrows come over and consult on Scott's case. We loved that recommendation,even though the MD today gave us great confidence. We have a ton of questions for that barrows guy!
Here's what's new for today:
1. Speech therapy placed a one way valve (speaking valve) in today to test him out. This allows him to breath through the trach and out through his mouth. She left it in for 5 minutes and he did perfectly well. Soooo next week when they are able to place the smaller tracheostomy tube in, they will be able to place a speaking valve in it. They also mentioned that he isn't able to smell right now because there is no air passing through his nasal passages, but once they put the speaking valve in, he will be able to smell and we will be able to start stimulating his brain through smell. Oh... The one way valve allows him to breathe in through the trach tube and out through his nose.
2. They have taken out the central IV line and have replaced it with a peripheral IV line.
3. They took out the Foley catheter and put a condom catheter on. They may still have to straight cath him due to neurogenic bladder,but it will decrease the risk for infection. His bladder muscles will have to be re-trained along with everything else.
4. They just did a follow up CAT scan. We will get the report tomorrow.
5. Scott's dad, Mickey, brought in a fan today to help keep his temperature under control. They had one in the ICUS, but they don't have them here. They allowed us to bring one in. He seems to be more settled and no longer sweating.
6. They will remove the trach as soon as he is safe to do so. He needs to be able to swallow and manage his secretions. They will test his swallowing once he gets the speaking valve in.
7. He has lost 12 pounds, so they are increasing his calories.
8. His wounds are progressing quite well. Once the staples begin to "float", they will remove them.
9. Rehab placed boots on him today and will alternate them on and off every 2 hours to protect his heels from pressure sores and to protect him from "drop foot". PT and OT will be here M-F and will focus on increasing his awareness with his environment, strengthening extremities and core, and building his activity tolerance. Today, he was able to sit unsupported. He fatigues very quickly and begins drifting to the right. He is responding better to commands today, including visual tracking and mouth movements. They had me kneel next to Scott while he was sitting on the edge of the bed, and talk to him. He turned his eyes toward me. Yeah! I then placed my hand next to him, and asked him to touch my hand. Nothing. They then brought Ashley in to repeat the same instructions. He immediately reached for her hand and followed her commands. Ashley is worried that Scott may not remember who she is, so this was a bit encouraging. We are taking it that he knows and remembers that she is special to him.
They told us today that he may have to go to a sub-acute setting for 2-3 weeks before going to Barrows, if he improves medically but is not able to tolerate 3 hours of therapy per day. Whatever is the most successful course is good with us. They will begin sitting him up in a chair daily increasing his tolerances to a maximum of 2 hours. 2 hours is the bed sore limit. They will put him in a Barton chair, which has an incline backward, in order to keep him from falling forward out of the chair and it will provide support for his head. He gets exhausted very easily, but he seems to be resting much better today. They also said it is time to begin sensory stimulation. Phone calls to hear familiar voices, talking to him about things that might agitate him a little (in order to get a stronger response), music, photos, etc. Things that are familiar to him.
In my exhaustion and frustration yesterday, I forgot to thank Bishop King, Bishop Matthews, Scott Smith, President Forsberg, and Melynda King for coming by to give Scott and Ashley a blessing. We are beyond grateful! Also, we are very grateful for Mickey And Carol Moore, Scott's dad and step mom, who have been working tirelessly a and fervently to get all of the logistic things taken care of (police reports, insurance issues, etc.), thus allowing Ashley and I to focus on Scott himself and his medical needs. It has been a huge relief and blessing! Oh... I almost forgot.... When he was being transferred back to his bed after having his CAT scan done, he rolled himself over onto his side! It was so cool to see! So... all in all a much better day today! Yeah! "Talk to you again tomorrow!" Patti
1. Speech therapy placed a one way valve (speaking valve) in today to test him out. This allows him to breath through the trach and out through his mouth. She left it in for 5 minutes and he did perfectly well. Soooo next week when they are able to place the smaller tracheostomy tube in, they will be able to place a speaking valve in it. They also mentioned that he isn't able to smell right now because there is no air passing through his nasal passages, but once they put the speaking valve in, he will be able to smell and we will be able to start stimulating his brain through smell. Oh... The one way valve allows him to breathe in through the trach tube and out through his nose.
2. They have taken out the central IV line and have replaced it with a peripheral IV line.
3. They took out the Foley catheter and put a condom catheter on. They may still have to straight cath him due to neurogenic bladder,but it will decrease the risk for infection. His bladder muscles will have to be re-trained along with everything else.
4. They just did a follow up CAT scan. We will get the report tomorrow.
5. Scott's dad, Mickey, brought in a fan today to help keep his temperature under control. They had one in the ICUS, but they don't have them here. They allowed us to bring one in. He seems to be more settled and no longer sweating.
6. They will remove the trach as soon as he is safe to do so. He needs to be able to swallow and manage his secretions. They will test his swallowing once he gets the speaking valve in.
7. He has lost 12 pounds, so they are increasing his calories.
8. His wounds are progressing quite well. Once the staples begin to "float", they will remove them.
9. Rehab placed boots on him today and will alternate them on and off every 2 hours to protect his heels from pressure sores and to protect him from "drop foot". PT and OT will be here M-F and will focus on increasing his awareness with his environment, strengthening extremities and core, and building his activity tolerance. Today, he was able to sit unsupported. He fatigues very quickly and begins drifting to the right. He is responding better to commands today, including visual tracking and mouth movements. They had me kneel next to Scott while he was sitting on the edge of the bed, and talk to him. He turned his eyes toward me. Yeah! I then placed my hand next to him, and asked him to touch my hand. Nothing. They then brought Ashley in to repeat the same instructions. He immediately reached for her hand and followed her commands. Ashley is worried that Scott may not remember who she is, so this was a bit encouraging. We are taking it that he knows and remembers that she is special to him.
They told us today that he may have to go to a sub-acute setting for 2-3 weeks before going to Barrows, if he improves medically but is not able to tolerate 3 hours of therapy per day. Whatever is the most successful course is good with us. They will begin sitting him up in a chair daily increasing his tolerances to a maximum of 2 hours. 2 hours is the bed sore limit. They will put him in a Barton chair, which has an incline backward, in order to keep him from falling forward out of the chair and it will provide support for his head. He gets exhausted very easily, but he seems to be resting much better today. They also said it is time to begin sensory stimulation. Phone calls to hear familiar voices, talking to him about things that might agitate him a little (in order to get a stronger response), music, photos, etc. Things that are familiar to him.
In my exhaustion and frustration yesterday, I forgot to thank Bishop King, Bishop Matthews, Scott Smith, President Forsberg, and Melynda King for coming by to give Scott and Ashley a blessing. We are beyond grateful! Also, we are very grateful for Mickey And Carol Moore, Scott's dad and step mom, who have been working tirelessly a and fervently to get all of the logistic things taken care of (police reports, insurance issues, etc.), thus allowing Ashley and I to focus on Scott himself and his medical needs. It has been a huge relief and blessing! Oh... I almost forgot.... When he was being transferred back to his bed after having his CAT scan done, he rolled himself over onto his side! It was so cool to see! So... all in all a much better day today! Yeah! "Talk to you again tomorrow!" Patti
Subscribe to:
Posts (Atom)